|
||
The World Alliance for Breastfeeding Action (WABA) is a global network of individuals & organisations concerned with the protection, promotion & support of breastfeeding worldwide. WABA action is based on the Innocenti Declaration, the Ten Links for Nurturing the Future and the Global Strategy for Infant & Young Child Feeding. WABA is in consultative status with UNICEF & an NGO in Special Consultative Status with the Economic and Social Council of the United Nations (ECOSOC). |
 What is LAM? What is LAM?
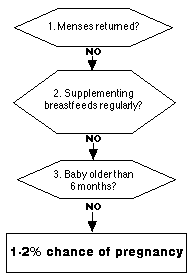
The Lactational Amenorrhea Method (LAM) When is LAM no Longer Effective? Family Planning for the Breastfeeding Woman Breastfeeding Habits that Improve LAM Frequently Asked Questions about LAM The Lactational Amenorrhea Method (LAM) It is a well known fact that breastfeeding suppresses a woman's fertility in the early months after delivery. However, many women do not feel comfortable relying on breastfeeding as a form of birth control because they have been told it is unreliable, or perhaps because they know someone who became pregnant while breastfeeding. The Lactational Amenorrhea Method (LAM) was created to allow women to safely rely on breastfeeding as a family planning method. Based on scientific research, the method uses three measures of a woman's fertility: 1) the return of her menstrual period, 2) her patterns of breastfeeding, and 3) the time postpartum. Who can use LAM? A woman can use LAM if: 1. her menstrual period has not returned since delivery (Bleeding or spotting during the first 56 days is not considered menstrual bleeding.) AND 2. she is breastfeeding her baby on demand, both day and night and not feeding other foods or liquids regularly (Occasional tastes of foods or other liquids are permitted, but they should never replace a feeding at the breast.) AND 3. her baby is less than six months old. When all three of these conditions exist, she has less than a two percent chance of becoming pregnant. However, the woman is encouraged to begin using a complementary family planning method when any of the three conditions changes, or whenever she chooses.
Scientific studies conducted around the world by the Institute for Reproductive Health and other organizations have proven that when used correctly, LAM is an effective, safe, convenient short-term way for breastfeeding women to delay pregnancy.
** Study conducted by Family Health International.
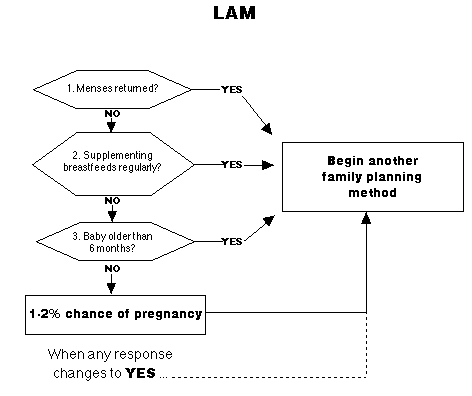
A woman who chooses to rely on LAM should be advised that the method is short-term (up to six months) and is no longer effective when any one of the three criteria changes. The LAM user should be counseled to use another contraceptive method for continued protection when: 1. Her menstrual periods return. 2. She begins feeding her baby other liquids or foods regularly, or her baby sleeps through the night. 3. Her baby is older than six months. Any one of these changes will reduce LAM's high efficacy. At this time, the LAM user should be counseled about complementary family planning methods that do not interfere with breastfeeding. Medical conditions when LAM would not be advisable LAM should not be used under the following conditions:
AIDS or confirmed HIV+. The HIV virus can be passed through breastmilk. According to the World Health Organization, if a safe alternative to breastfeeding is available and affordable, a woman who is HIV+ or has AIDS should be informed of the risks of breast and bottle feeding. Active tuberculosis. Tuberculosis does not spread through breastmilk but through direct contact with the mother. If the mother has an active case of tuberculosis, breastfeeding increases the risk of infection due to the frequent and intimate contact with the infant. This page was adapted from the original web site of the Institute for Reproductive Health, a project funded by the United States Agency for International Development (USAID) under the terms of Cooperative Agreement DPE-3061-A-00-1029-00. Information (photos excluded) and publications may be reproduced, adapted, and disseminated without permission, provided the Institute for Reproductive Health is acknowledged and the material is distributed free of charge, or not for profit. The LAM section was originally developed by Shirley Coly Photograph on this page by Noureddine El-Warari.
|
 |
World Alliance for Breastfeeding Action |
||
| Site Map | PO Box 1200, 10850 Penang, Malaysia | Tel: 604-6584816 | Fax: 604-6572655 | E-mail: waba@waba.org.my | http://www.waba.org.my | |